Individuals with PWS suffer from a variety of digestive and gastrointestinal issues (GI), some of which can lead to surgery. Here, we focus on data from the Global PWS Registry to provide information on the prevalence of gastroparesis (delayed stomach emptying), as well as the frequency and types of GI surgeries in PWS.
Gastroparesis occurs when food doesn’t properly empty from the stomach into the intestinal track to continue the normal process of digestion. This step of stomach emptying is a coordinated effort where the vagus nerve stimulates the stomach to contract and squeeze food forward into the intestine. Without this stimulation, the stomach is basically paralyzed, and the food just sits in the stomach. For those who develop gastroparesis, it is a chronic condition, and without continued management, flare ups can lead to further complications. Fortunately, there are a variety of treatments that can help reduce the severity and frequency of flare ups.
Individuals with PWS are at high risk for gastroparesis compared to the general population. Additional risk factors for gastroparesis include diabetes and the use of certain antidepressants.
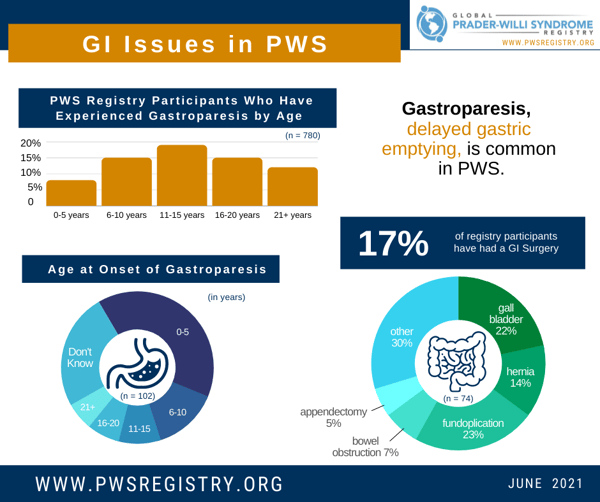
Within the Global PWS Registry, the percentage of participants with a diagnosis of gastroparesis ranges by age group. Overall, among all age groups combined, 13% of registry participants have gastroparesis. However, the number is highest among those in the 11-15 age group, where more than 19% of participants suffer from this problem. Of those who have gastroparesis, more than 50% were diagnosed by age 10, although there are individuals who developed this problem as adults.
Symptoms of gastroparesis can include heartburn, acid reflux (when stomach contents come back up into the esophagus), vomiting undigested food, bloating, and stomach pain, with impacts on appetite and regulation of blood sugar levels. Without treatment to move the food along out of the stomach, gastroparesis can lead to bacterial growth in the stomach, as well as hardening of the undigested food into what is called a bezoar. A bezoar is a hardened mass of partially digested or undigested material in the intestinal tract. It usually forms in the stomach and then moves into the intestines. Smaller bezoars can eventually pass through the digestive track on their own. However, if large enough, a bezoar can cause an intestinal blockage that requires surgical removal.
Among participants in the Global PWS Registry, bezoar surgery is not highly reported, but there are a handful of cases. However, 17% of registry participants have undergone some type of GI surgery. Of those who have had a GI surgery, the three most common procedures are gallbladder surgery/removal, hernia repair, and fundoplications. Fundoplications aim to improve GERD (gastroesophageal reflux disease), which is when stomach acid comes up into the food pipe, causing irritation and burning.
If you suspect that your loved one with PWS is experiencing gastroparesis or frequent acid reflux and heartburn, please consult your physician or a GI specialist for more information on testing and diagnosis.
For more information on the Global PWS Registry, please visit pwsregistry.org or email the Registry here.








